April 5, 2026
Before Something Goes Wrong on the Trail
Most people heading into the backcountry are not climbing glaciers or pushing into extreme environments. They are day hikers, weekend backpackers, families, and people looking to spend time outside on well-traveled trails. The terrain feels familiar, the weather seems manageable, and the assumption is that if something goes wrong, help is not that far away.
That assumption is where problems begin.
Even in these everyday environments, it does not take much for a situation to turn. A bad step on loose rock, a sudden change in weather, dehydration creeping in over a few hours, or someone pushing a little too hard on the way out. Once someone is hurt, you are no longer just hiking. You are now responsible for managing a problem with limited gear, limited support, and no immediate backup.
A lot of people also have a Hollywood version of search and rescue in their heads. They picture a fast response, a helicopter overhead, and trained professionals arriving almost immediately. That is usually not how it works. In many cases, search and rescue has to be notified, volunteers have to assemble, information has to be gathered, your location has to be narrowed down, conditions have to be evaluated, and then a team has to physically make its way to you. They also have to decide whether it is safe for them to come in at all. That process takes time. Sometimes it takes hours. Sometimes it takes much longer than people expect.
That reality matters because it changes the whole way you should think about backcountry emergencies. If you are a few miles in on a trail, you need to understand that you and the people around you may be the only care available for a while. In 16 years of teaching outdoor wilderness skills, I have found that very few people out there have any real medical training beyond CPR. I ask this in class all the time. In a group of 10 to 20 people, maybe 1 hand goes up. Sometimes 2. That means the vast majority of people on the trail are hoping nothing serious happens because they do not have much to fall back on if it does.
CPR is still worth knowing, but people also need to be honest about its limitations in the backcountry. If someone goes into cardiac arrest miles from the trailhead, you are not going to realistically perform continuous CPR until rescuers arrive. That is not physically sustainable in rough terrain over long periods of time, especially if help is far away. CPR has its place, but it is not the same thing as being prepared to handle a wilderness medical problem. If you want to be of real value when something goes wrong, you need training that goes beyond CPR and helps you assess, manage, and stabilize a patient in the environment you are actually in.
This is where Wilderness First Aid training becomes relevant. Not as a checkbox or a certification, but as a way to slow things down, think clearly, and work through a situation in a structured way.

You won’t always have perfect gear. Use what you have and keep moving.
What Wilderness First Aid Actually Teaches
At its core, Wilderness First Aid is about decision making and patient assessment in an environment where you cannot just call for help and expect it to arrive quickly. It gives you a framework to evaluate what is going on, prioritize what matters, and take action with what you have on hand.
You are not learning to be a paramedic. You are learning how to manage a situation long enough to stabilize someone and figure out what to do next. That might mean treating and continuing, treating and staying put, or beginning an evacuation.
The most valuable part of that training is not the gear or even the specific techniques. It is the process.
It also teaches you how to think when things are not clean or obvious. Most real situations do not present themselves in a textbook way. People do not always give clear answers, injuries overlap, and conditions change as you are working through them. Wilderness First Aid gives you a way to work through uncertainty instead of freezing or jumping to the wrong conclusion.
Another piece that often gets overlooked is improvisation. In the backcountry, you are rarely working with a perfect medical kit. You are using what you have. That might mean turning a jacket into insulation, a trekking pole into part of a splint, or a backpack into a way to help move someone. The training builds the ability to look at your environment and your gear differently so you can solve problems instead of getting stuck on what you do not have.
It also reinforces the idea that your job is not to fix everything. Your job is to prevent the situation from getting worse and to make good decisions about what happens next. That shift in mindset alone changes how people respond under pressure and gives them a much better chance of handling a situation the right way.
It is also worth understanding that these are not just backcountry skills. The same way you assess and manage a patient on a trail is the same way you would approach someone in a parking lot, at your house, or at the scene of a car accident. The environment changes, but the process does not. If something happens in front of you, you are the first one there whether you planned for it or not. If you have a few minutes to respond and it takes emergency services longer to arrive, those first decisions carry weight. This kind of training carries over into everyday life in a very real way, and that is where it becomes even more valuable.

This is where people learn how to think, not just what to do.
Scene Assessment: Slowing Yourself Down Before You Act
Before you touch the patient, before you start focusing on them, and before you do anything else, you need to look at what is happening around you and understand why they are in that situation in the first place.
Scene assessment starts with a simple question. Is this situation safe for me and everyone else involved?
That sounds obvious, but this is where people often rush in and make things worse. Loose rock, unstable slopes, incoming weather, lightning, wildlife, fast moving water, traffic near a trailhead, or even other hikers moving through the area can all turn one patient into multiple problems. There can also be hazards people do not immediately think about, such as downed power lines, vehicle accidents on mountain roads, fuel spills, or areas with poor air quality and limited oxygen. If your buddy suddenly collapses in a confined space, charging in after them without thinking may get you hurt too. Sometimes the most dangerous part of the situation is not the injury itself, but the environment around it.
This is one of the hardest things for people to do because the natural instinct is to move fast and help. But helping without thinking is not always helping. If you go down trying to rescue someone, you have now made the problem bigger and put even more pressure on everyone else.
You also want to understand what actually happened. How the injury occurred will guide everything you do next. A simple fall on flat ground is very different from someone tumbling down a slope, taking a hit to the head, getting struck by lightning, or being involved in a vehicle rollover on the way to the trail. The story of what happened starts shaping your decisions before you ever begin hands-on care.
At the same time, you should be paying attention to anything that does not fit. Does the scene make sense? Is there something out of place? If your only visible patient is a smaller female hiker but you notice a larger boot, a second pack, or gear that clearly does not belong to her, there may be someone else involved. You may not be dealing with a single patient. These small details can completely change how you approach the situation. You would be surprised how much people miss when they are under stress.
Scene assessment is not just about spotting hazards, it is about understanding the situation as a whole. Are you dealing with a single injury, or is there something else going on that has not been identified yet? Is there an ongoing danger that could hurt others? Do you need to move the patient, move yourself, or stay where you are and work carefully? Those first few seconds of observation shape everything that follows.
Taking a few extra seconds here to slow yourself down and think clearly will put you in a much better position than reacting fast and guessing.

You don’t rush into the problem. You take a second and understand it first.
AVPU: A Quick Check Before You Dive In
Right after you assess the scene and determine it is safe to approach, you want a quick read on the patient’s mental status. This does not take long and it tells you a lot right away.
AVPU is a simple way to do that.
A is for Alert. The patient is awake, aware, and able to respond clearly, and you confirm this by talking to them. Ask simple questions like who they are, where they are, and what happened, and listen for clear, appropriate answers. You are looking for responses that make sense, not confusion or delayed reactions. Pay attention to how they act as well, including eye contact and focus, not just what they say. If they can carry on a normal conversation, that tells you their airway is open, they are breathing, and their brain is functioning well enough to communicate.
V is for Verbal. The patient is not fully alert, but they will respond when you speak to them. You may have to repeat yourself or speak louder, and their responses are often slow, confused, or incomplete. They might answer incorrectly, mumble, or say things that do not quite make sense, but they are still reacting to your voice. They may open their eyes, turn their head, or try to speak when prompted, even if it is not clear or accurate. This tells you they are responsive, but something is not right and needs attention.
P is for Pain. The patient does not respond to your voice, but they will react when a painful stimulus is applied. This should be something controlled and purposeful, such as a sternal rub or a firm pinch to the shoulder or trapezius. A sternal rub is done by pressing your knuckles into the center of the chest and rubbing firmly back and forth to create a strong pain response. You are not being gentle here, you are trying to get a reaction. You are looking for any response, not just words, including pulling away, grimacing, or attempting to move. Even a small reaction tells you the brain is still processing stimuli at some level. This is a sign of a more serious condition and should be taken seriously.
U is for Unresponsive. The patient is not responding at all, with no reaction to voice and no reaction to pain. They will not open their eyes, move, or make any sounds when stimulated. This is a serious condition and should be treated as an immediate life threat. At this point, you move quickly into your ABCDE assessment with a strong focus on airway, breathing and blood loss.
This is not a detailed neurological exam. It is a quick snapshot that helps you understand how serious the situation might be. Someone who is alert and talking is in a very different situation than someone who only responds to pain or not at all.
It also gives you a baseline. If their condition changes later, you have something to compare it to.

Start simple. Talk to them and see how they respond.
The ABCDE Approach
Once you move in, you need a way to prioritize. That is where the ABCDE approach comes in. It gives you a clear order of operations so you are not bouncing around or missing something that could cost someone their life.
Before you begin, take a second to put on your PPE (personal protection equipment). If you have a first aid kit in your pack, you should have medical grade gloves. This is the time to glove up. You are about to make contact with the patient, and protecting yourself matters just as much as helping them.
If you are not sure what should be in your kit, we break it down in our Wilderness Medical Kit Guide.
This initial assessment should be quick. Realistically, you should be able to move through ABCDE in about 30 seconds to 2 minutes. It is not meant to be a deep dive, it is a rapid check to identify immediate threats. And it does not happen just once. You continue to cycle through it as you manage the patient because things can change quickly, especially breathing and circulation.
If a patient is talking clearly to you, you have already answered two major questions. Their airway is open and they are breathing. That alone gives you a lot of information before you even begin.
As you move through ABCDE, you do not wait to fix problems. If you find a life threat, you handle it immediately before moving on. This is not a checklist you complete at the end. It is something you work through while actively managing the patient.
A is for Airway. If the airway is not open, nothing else matters. You are checking to make sure there is a clear path for air to move in and out. This could be blocked by the tongue, blood, vomit, swelling, or a foreign object. If the airway is not open, you address that immediately.
B is for Breathing. Once the airway is open, you are looking at how well they are breathing. Just because the airway is open does not mean they are breathing effectively. Watch the rise and fall of their chest. Is it steady and normal, too fast, too slow, shallow, or not there at all? Look for signs of chest injury or distress, and listen for abnormal sounds if you are close enough. You are making sure oxygen is actually moving. This is one you keep coming back to, because it can change fast.
C is for Circulation. This is where you look for bleeding first. Severe bleeding needs to be controlled right away. In a backcountry setting, that might mean direct pressure, packing a wound, or using a tourniquet.
If you do not immediately see blood, that does not mean it is not there. You need to physically sweep the patient with your hands, checking their entire body. As you move your hands, check your gloves after each section for blood. You are not just looking, you are feeling. Check under the body if needed, but try to move them as little as possible, especially the head and neck.
Once you have ruled out major bleeding, you can quickly check pulse and skin condition to get a general sense of circulation. You are not doing a full medical workup here, you are looking for obvious signs that something is off, like weak or absent pulse or pale, cool, or clammy skin.
This step takes more time than airway and breathing, but it should still be done efficiently.
D is for Disability. This is a quick check of mental status and neurological function. You are building off the AVPU assessment you already performed and looking for any changes or abnormalities. Is the patient still alert, or are they becoming confused, slow to respond, or less responsive over time? You are also looking for obvious neurologic signs such as unequal pupils, slurred speech, unusual behavior, or loss of coordination. These can point to problems like head injury, lack of oxygen, dehydration, or altitude related issues. This is another area you continue to reassess, because changes here can happen quickly.
By the book, D stands for Disability, but in the real world people will often notice a major Deformity during this step. If you see something obvious like a severely angulated limb or a clear dislocation, it is hard to ignore. That is not technically what this step is meant for, but if you know what you are doing and can address it quickly without creating additional problems, it may be appropriate to handle it. Just understand that life threats always come first, and you do not let something like a broken bone distract you from airway, breathing, or major bleeding.
E is for Environment. This is often overlooked, but it plays a major role in how a patient progresses. A patient who is stable can become unstable quickly if they are exposed to cold, wind, rain, or heat. Managing the environment around the patient is part of treating the patient. One of the first things to think about is getting them off the ground. The ground will pull heat from the body faster than most people realize, even when it does not feel that cold. Put something under them like a jacket, pack, sleeping pad, or anything you have available to create insulation. People forget about this all the time, and it can make a big difference.
The strength of ABCDE is that it keeps you focused. You are not guessing what to do next. You are working through a system that prioritizes the biggest problems first while constantly reassessing as the situation evolves.
Before wrapping this up, it is worth mentioning another approach you may hear about called the MARCH protocol. This comes from military medicine and is built around the types of injuries they commonly deal with, especially severe trauma and massive bleeding. It can also apply in certain civilian situations, such as serious car accidents or high impact injuries.
The MARCH protocol stands for Massive hemorrhage, Airway, Respiration, Circulation, and Head injury or Hypothermia. The key difference is that massive bleeding is addressed first, even before airway, because uncontrolled hemorrhage can lead to death very quickly. This requires fast action and the ability to recognize what is happening in front of you.
For most backcountry situations, ABCDE is a solid and reliable approach. The MARCH protocol is just another tool to be aware of when the situation involves severe trauma.
That is a deeper topic for another time, but it is worth knowing it exists.
If you want to go deeper on this, check out the full breakdown of the MARCH Protocol where we walk through how it applies in real world scenarios.

If you find a life threat, you fix it before moving on.
If you want something simple you can carry with you, I put together a one page field reference that walks through AVPU and ABCDE step by step. You can download it here. AVPU and ABCDE Patient Assessment Guide
The Secondary Assessment: Finding What You Missed the First Time
Once you have worked through your primary assessment and addressed any immediate life threats, you can slow things down slightly and take a more detailed look at your patient.
This is where you start looking for everything that was not immediately obvious. Not every injury is going to jump out at you right away. Some problems take a minute to show themselves, and others get missed because your focus was on keeping the patient alive.
The goal here is simple. You are trying to find everything that is wrong before it becomes a bigger problem.
This is typically done as a head to toe check. You are using both your eyes and your hands, not just looking but feeling for anything abnormal. Deformities, swelling, bruising, tenderness, instability, or anything that does not feel right.
Start at the head and work your way down. Check the scalp, face, and neck. Look for bleeding, deformities, deformities, bone fractures, or other signs of trauma. Move to the chest and ribs, feeling for pain, instability, or uneven movement. Check the abdomen for tenderness or rigidity. Move through the pelvis, then down each arm and leg, checking joints, bones, and soft tissue.
A good way to think about this is to imagine a scanner slowly moving down the body from head to toe. It does not jump around or skip sections. It moves steadily, covering everything in its path. That is exactly what you are doing with your eyes and your hands. You are moving in one direction, staying focused on the section you are in, and fully checking it before moving on.
If you rush this or bounce around, you will miss things. Staying methodical is what keeps you from overlooking injuries that are not immediately obvious.
This is also a good time to check for things that can give you more information about the patient. Look for medical alert bracelets or necklaces. Check pockets or packs if appropriate. Sometimes the patient cannot tell you what is wrong, but there may be clues on them that can help guide your decisions.
You are also paying attention to how the patient reacts as you move through this. Pain, hesitation, or guarding can tell you just as much as what you see.

Once immediate threats are handled, slow down and work through the details.
This Is Where We Draw the Line
At this point, you have a way to assess a patient, find problems, and start making decisions. Once you find something, you treat it. Prioritize the most serious issues first, then work your way down. Stay disciplined. Not everything that looks bad actually is bad, and not everything that is dangerous looks dramatic.
A good example is a face wound. They bleed a lot and can look severe fast. That can pull your attention in and make you think it is the biggest problem. Meanwhile, a swollen and painful thigh might not look nearly as dramatic, but it can be far more serious. You have to think through what you are seeing and not get distracted.
From here, the rabbit hole gets deep quickly. We could go into how to treat burns, fractures, dislocations, bleeding, head injuries, environmental problems, and everything in between, but at that point we are not writing a blog anymore, we are writing a book. This is where we stop.
If you want to actually know how to treat the problems you are finding, that comes from hands-on training and time spent doing it, not just reading about it.

There is a lot that happens between basic care and something like this.
Why This Matters for Everyday Hikers
Most people heading out on an adventure are not carrying advanced medical kits, and they are not expecting to manage serious injuries. They are thinking about the weather, the trail, maybe what they packed for lunch, and how long it will take to get back to the car. It is a normal day. That is the mindset almost everyone brings with them, and most of the time, that mindset works just fine.
But the problem is not the normal day. The problem is how quickly a normal day can turn into something else.
It does not take much. One bad step on loose rock, one misjudged crossing, one person pushing just a little too hard on the way out. What was a simple hike a few minutes ago is now a situation that has to be managed. Distance starts to matter. Time starts to matter. Weather starts to matter. The same trail that felt easy on the way in suddenly feels very different on the way out when someone cannot move the way they need to.
A twisted ankle five miles from the trailhead is not just a twisted ankle. It is now a mobility problem, which turns into a timing problem, which can turn into an exposure problem if things start to stack up. A minor cut that gets ignored can become something worse if it is not cleaned and managed properly. Someone who says they feel a little off at elevation might be dealing with dehydration, exhaustion, or something more serious that has not fully shown itself yet.
A lot of the time, these situations do not look dramatic at first. It is usually a slow shift. Things start to feel off. Small problems start to build. And if no one steps in and manages it early, that is when it turns into something bigger.
But not always.
Sometimes it is immediate and it is serious. Someone takes a hard fall and does not get up. Someone hits their head. A leg is clearly broken. Someone collapses without warning. When that happens, there is no easing into it. The situation is right in front of you, and it is not going to wait for you to get comfortable. That is the moment where everything changes.
You are no longer just out on a hike. You are the one responsible for what happens next. There is no one else stepping in to take over. No one is coming around the corner to handle it for you. It is on you and whoever is with you to figure it out and start doing something.
This is where most people struggle. Not because they are not capable, but because they do not have a process. They hesitate, they second guess, or they focus on the wrong thing because it looks worse than it actually is while something more serious gets missed. Without a structure to fall back on, people tend to react instead of think.
Wilderness First Aid gives you that structure. It gives you a way to step into that moment and take control of it instead of hoping it resolves itself. You can slow things down, work through the problem, and make decisions based on what is actually happening instead of what it feels like in the moment. And that shift, from reacting to thinking, is what makes the difference.
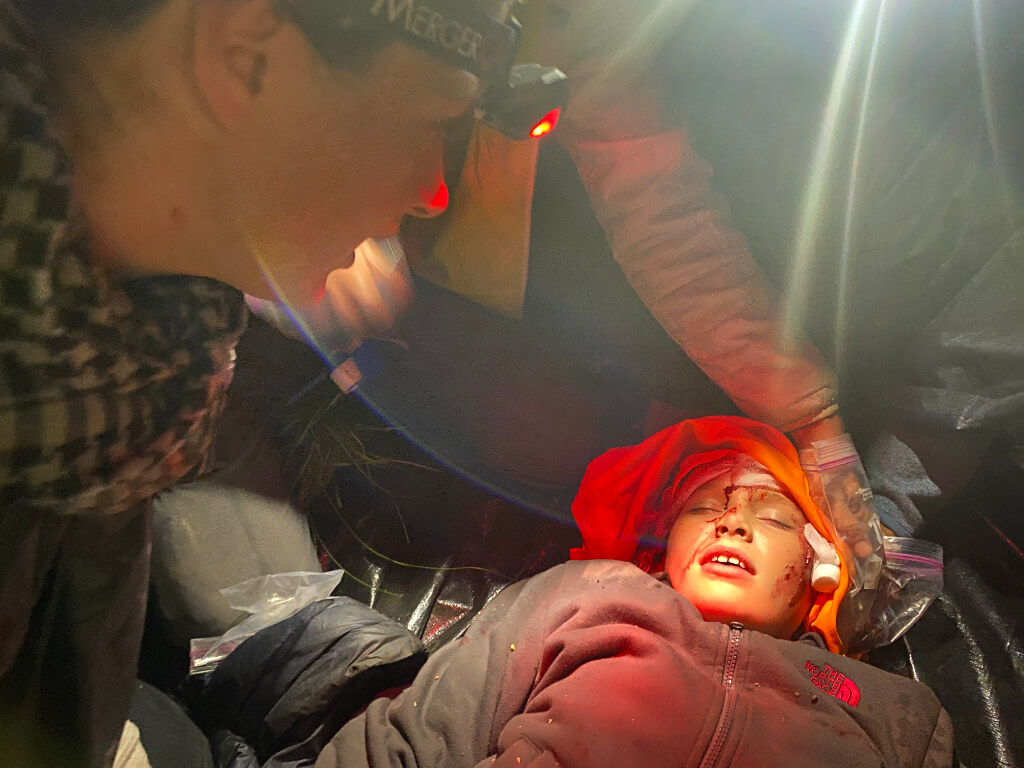
This is where training shows up or it doesn’t.
The Reality of WFA and Going Further
Wilderness First Aid is a strong starting point. It gives you the ability to recognize problems, prioritize care, and make decisions that can keep someone stable in a remote setting. For most day hikers and weekend adventurers, that alone puts you ahead of the majority of people on the trail. You go from being someone who hopes nothing happens to someone who can step in and actually do something when it does.
It is also a very practical course for most people. It is typically a 2 day training, it is accessible, and it fits into the reality of busy schedules. For many people, that is exactly what they need, and it is far better than having no training or relying on basic CPR alone. We do include hands-on components and small scenarios in our courses, but there is only so much you can realistically cover and practice in that amount of time.
At the same time, it is still a starting point.
A short course can give you the framework and expose you to the concepts, but it does not give you depth. It does not give you enough time to truly build confidence, and it does not give you enough repetition to make those skills automatic. When things get real, people do not perform based on what they vaguely remember. They fall back on what they have practiced. You can and should continue practicing these skills on your own after the course, but there is a difference between running through something at home and working through a problem in a real environment with pressure and variables you cannot control.
There are layers to this that go far beyond the basics. Patient assessment is not something you do once and move on from. It is something you repeat, refine, and adjust as the situation changes. Small details start to matter more. Subtle changes in mental status, breathing, or circulation can tell you that something is getting better or getting worse. If you are not used to looking for those changes, you will miss them.
Then there is the reality of time. In the backcountry, you are not dealing with a quick handoff to EMS. You might be managing someone for hours. In some cases, longer. That changes everything. Now you are thinking about how to keep them warm, how to keep them hydrated, how to manage pain, how to move them, or whether moving them is even the right call. These are not one-time decisions. They evolve as the situation unfolds.
Evacuation is its own problem. Getting someone out of the field is rarely simple. Terrain, weather, distance, and the condition of the patient all play a role. You have to think through what is realistic, what is safe, and what your group is actually capable of doing. That level of decision making is hard to teach in a short course because it requires time, experience, and the chance to work through mistakes in a controlled setting.
That is where more advanced training comes in. Not because the basics are not useful, but because building real capability takes time. It takes repetition. It takes being put in situations where you have to think, adapt, and apply what you know under pressure.
If you want to move beyond just having an idea of what to do and get to the point where you can actually handle these situations with confidence, you need more than a quick introduction. You need time in the field, hands-on training, and the chance to work through problems until the process becomes second nature.
That is where Wilderness First Responder training comes in.
It takes everything you learned at the basic level and builds on it through repetition, longer scenarios, and more realistic problem solving. You are not just learning what to do, you are practicing how to think, how to adapt, and how to manage a patient over time. You start to see how situations evolve, how small details matter, and how to stay ahead of problems instead of reacting to them.
That is where confidence is built.

Stabilized for now. The work does not stop here, this is where real decision making begins.
Why Wilderness First Aid Training Matters in the Real World
Most people do not plan to use any of this. They head out for a hike expecting a normal day, and most of the time, that is exactly what they get. That is why it is easy to push this kind of training off or assume it is something you will deal with later.
But emergencies do not wait for you to feel ready.
When things shift, they shift fast. One moment you are moving down the trail, and the next you are standing there trying to figure out what just happened and what you are supposed to do about it. That gap between those two moments is where people either step in or freeze.
Having a structured way to assess a situation, prioritize what matters, and take action with what you have is what closes that gap. It gives you something to fall back on when your brain wants to speed up or shut down. It allows you to slow things down, think clearly, and move forward with purpose instead of guessing.
Wilderness First Aid is not about turning you into a medical professional. It is about making sure you are not helpless when someone needs you. It is about being able to step into a situation and do something useful instead of standing on the sidelines hoping someone else takes over.
And whether that moment happens five miles into the mountains, on the side of the road, or in your own backyard, the skill set is the same. Wilderness First Aid and Wilderness First Responder training are not just for the wilderness. What they really teach you is how to think, how to assess, and how to act when you do not have a fully stocked ambulance sitting right in front of you. You learn how to improvise, how to use what you have, and how to manage a situation when help is not immediate.
That is what makes this training valuable, no matter where you are.

Moving a patient is rarely simple, even when you know what to do.
All photos were taken during Wilderness First Aid and Wilderness First Responder training at The Survival University.

About the Author
Jason Marsteiner is the founder and lead instructor at The Survival University, where he’s turned his obsession with staying alive into a mission to teach real-world survival skills. Forget fancy gear, Jason’s all about the know-how that gets you through the wild or a city crisis. A published author of Wilderness Survival Guide: Practical Skills for the Outdoor Adventurer, he’s distilled years of hard-earned wisdom into lessons anyone can use.
Raised in Colorado’s rugged mountains, Jason’s survival chops were forged in the wild—from Missouri forests to Arizona deserts to Costa Rican jungles. He’s navigated it all with next to nothing, earning creds like Wilderness First Responder (WFR) and SAR tracking along the way. He’s trained thousands to keep cool when 911’s out of reach, proving survival’s not just for grizzled adventurers, it’s for hikers, parents, and city slickers alike.
Jason’s mantra? Everyone should make it home safe. When he’s not running courses, he’s designing knives, mentoring newbies, or chilling in the city like the rest of us, always sharpening the skills that turn panic into power.
